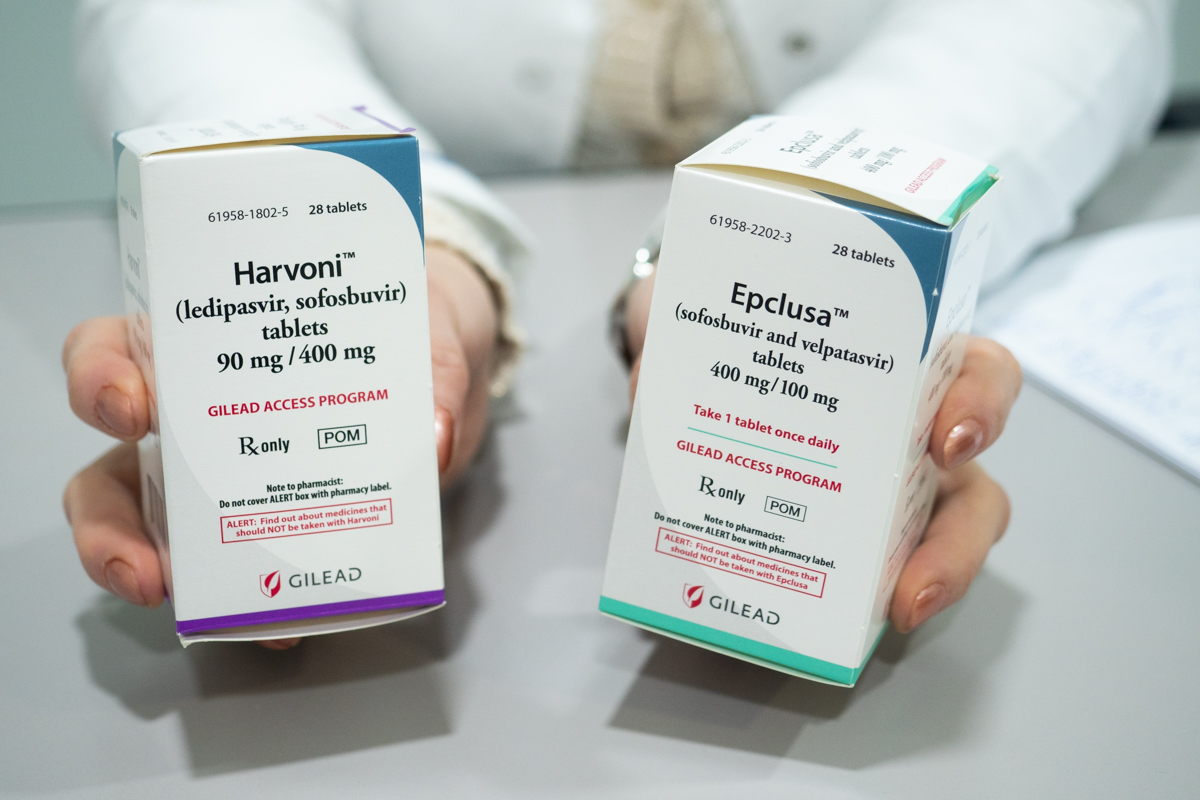
Tibilsi, Georgia, 2018. © Gemma Taylor/Make Medicines Affordable
On 7 February 2022, during Thailand’s National Health Security Board meeting, a representative from the Thai Network of People Living with HIV/AIDS (TNP+) submitted a proposal to remove barriers to HCV treatment to Anutin Charnvirakul, the Minister of Public Health and the Health Security Board’s chairman.
TNP+ President Apiwat Kwangkaew noted that sofosbuvir and velpatasvir (SOF/VEL), an oral, once-daily 12-week HCV treatment which cures at least 95% of people, has been included in the National Health Security scheme since January 2021, saying that:
“…We still face access problems, even though the medicine is procured and in stock.”
He explained that eligibility criteria, requirements for complicated pre-treatment diagnostic tests, and that HCV treatment be administered by a specialist – which often involves travel to faraway central or provincial hospitals – have delayed access, allowing the illness to worsen while the drugs to treat it are expiring. TNP+’s proposal addresses these issues, by broadening eligibility, simplifying diagnostic testing, and allowing trained doctors at community health centres to prescribe SOF/VEL, with the aim to expand treatment access to all people living with HCV.
The high price of SOF/VEL is still a barrier, although Thailand was eventually included in Gilead’s voluntary license (VL) in September 2017, after Malaysia issued a government use license for SOF (which Gilead priced at US $12,000 per treatment course).
Apiwat noted that “Only one generics company from India has registered SOF/VEL in Thailand, resulting in a market monopoly – and high prices (US $650 per 12-week treatment course).”
Although the VL allows Thailand to import generic versions of SOF/VEL from other licensees and produce its own versions, the price for SOF/VEL remains unacceptably high, because only one licensee has filed for and obtained approval to market their product in Thailand. Chalermsak Kittitrakul, the Project Manager at AIDS Access Foundation, a policy-advocacy NGO for access to affordable medicines in Thailand, said:
“This has created another kind of monopoly because other licensees may not be interested in the Thai market, or want to avoid the long wait for filing and registering their products here. This allows the first company to enter the market without competition – which keeps prices high. Local manufacturing is a way out of this problem. Thailand’s Government Pharmaceutical Organisation (GPO) is going to get market approval for their generic SOF/VEL in Q3 2022; competition will help bring down Mylan’s price for SOF/VEL. Local manufacturing and/or importing generics from different sources creates price-lowering competition, and ensures access. The lesson from Thailand is that a VL is not enough – multinational pharmaceutical companies use VLs to create a good image for the public, not to promote actual access. Multiple sources, including local producers, are needed to ensure access.”